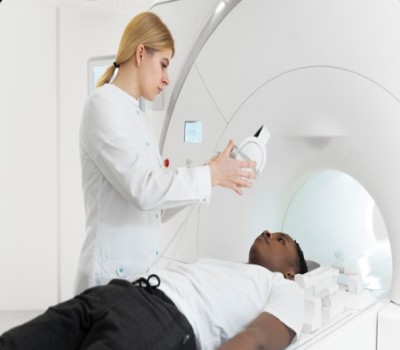
Hearing the word “radiation” can make anyone tense. People imagine pain, burns, and long hospital stays. But modern Radiation Oncology looks very different from what many people think. Today, radiation is planned with detailed imaging, delivered with millimeter-level precision, and checked again and again before the first treatment even begins.
The goal stays simple: treat the tumor effectively while protecting as much as healthy tissue as possible. That’s the idea behind targeted radiation and it’s why the process feels structured, calm, and surprisingly routine for many patients once they know the steps.
The first visit is about clarity, not rushing into treatment
Radiation usually starts with a consultation where the team reviews your diagnosis, scans, and treatment goals. In many cancers, radiation may be used to cure, control, or relieve symptoms—your plan depends on the cancer type, location, and stage. The most important part of this visit is decision-making: whether radiation is needed, what technique fits best, and how it will work alongside surgery, chemotherapy, or other treatments.
This step sets expectations early. It also helps patients do understand that radiation is planned, not improvised.
“Simulation” is the planning day where accuracy begins
Before any radiation session, you typically go through a planning appointment called simulation. This usually involves a CT scan in the exact position you will be treated in. The team may use custom supports (like a mask for head/neck or a cradle for body positioning) to keep your body steady in the same position each time. This planning step is a big reason modern radiation feels precise and repeatable.
Many patients ask about marks on the skin. Some centers use tiny tattoos, others use alternative markers. The purpose is simple: to line up the machine the same way every day so the radiation hits the intended area consistently.
The plan is built behind the scenes, and quality checks are real
After simulation, your radiation oncologist and medical physics team design the treatment plan. This is where “precision” truly happens—planning software maps the tumor and nearby sensitive organs, and calculates beam angles and dose patterns to treat the target while limiting exposure to normal tissues. Many centers also run formal checks before treatment begins, especially for complex plans, to make sure the plan matches safety and accuracy standards.
This is why treatment may not start the very next day. Planning takes time because it’s built to be exact.
Your first treatment day is usually simple and predictable
A typical external radiation session often feels like this: you check in, the team positions you exactly like your simulation, imaging may be done on the machine to confirm alignment, and then the radiation is delivered. You don’t feel the beam itself. The machine may move around you, and the team watches from a control room.
Most sessions are short, and you go home the same day. What matters more than the time is the consistency—showing up regularly and following instructions around skincare, hydration, and nutrition if advised.
Targeted radiation techniques—what “modern” really means
Modern radiation often uses methods that shape and direct dose with more control than older techniques. Two common terms patients hear are 3DCRT and VMAT.
3D CRT: precision across many angles
IMRT (intensity-modulated radiation therapy) is a type of radiation where thin beams of different intensities aim at the tumor from many angles. The intent is to reduce damage to healthy tissue near the tumor.
IMRT is often used when the tumor sits close to sensitive organs and the plan needs careful shaping.
VMART / Rapid Arc : high precision (duration of treat time reduced for selected cases)
SBRT (stereotactic body radiation therapy) is an external radiation technique that uses special equipment to position you and deliver radiation very precisely to body tumors. The total dose is divided into smaller doses given over several days, helping spare normal tissue.
SBRT is not “better” for everyone—it’s chosen when the tumor size, location, and motion (like breathing movement) allow safe high-precision treatment.
Brachytherapy: Internal Education
It is a form of radiation where we can use sealed radioactive sources which can be placed directly to the tumour or near to the tumour in the form of needle or catheter.
It is commonly used for cancers such as cervical, uterine, oral cavity cancers and soft tissue sarcoma. Treatment may be temporary or, in some cases, involve small, implanted sources.
Like other modern radiation techniques, brachytherapy is chosen based on tumour type, size, and location, it’s about selecting the right precision approach for the right situation.
Brachytherapy Advantages: We can spare the normal structures and can deliver high dose to the tumour with this method
Cancer treatment side effects—what to expect without fear
Side effects depend on where radiation is given, total dose, and individual sensitivity. Many side effects build gradually over days to weeks, rather than happening immediately.
Common experiences include fatigue, skin irritation in the treated area, and site-specific effects like throat soreness (if treating head/neck), bowel changes (if treating pelvis). Most teams give simple care instructions early—because managing side effects is part of the treatment plan, not an afterthought. Patient resources from radiation oncology groups also emphasize self-care steps and what symptoms to report.
Also important: side effects don’t automatically mean something is “going wrong.” Many are expected and treatable, but you should always report symptoms early so adjustments can be made.
You should follow proper instructions during the treatment (eg. avoid smoking/ soft drinks, following oral hygiene If you are getting radiation to oral cavity.
After radiation ends, follow-up is where healing continues
Radiation effects don’t stop on the last treatment day. Many tissues continue healing for weeks. That’s why follow-up appointments matter: your team checks symptom recovery, plans supportive care, and schedules scans at the right time (not too early, not too late) depending on cancer type.
This phase often feels like your body “settles.” Energy returns slowly. Skin calms down. Appetite improves. It’s not instant, but it is steady for many patients.
Final words
Modern Radiation Oncology is built around precision, planning, and safety. From simulation to planning to daily delivery, it runs like a system—because the goal is controlled, targeted radiation with carefully managed cancer treatment side effects, using modern techniques like 3DCRT and VMAT based on what fits your case best.
When patients understand the steps, fear reduces. The process becomes predictable. And that calm predictability is often the first part of healing.